You’ve been to the dentist. The X-rays came back clean. There’s no cavity. And yet, every time you bite down on the left side, there it is — that sharp, unmistakable jolt of pain. If this sounds familiar, you’re far from alone. In fact, it’s one of the most common dental complaints that doesn’t have an obvious answer at first glance.
The truth is, cavities are only one of many reasons a tooth can hurt. When biting pressure triggers pain but no decay is visible, your dentist needs to investigate deeper. Here are the most common hidden causes — and what you can do about each one.
1. Cracked Tooth Syndrome
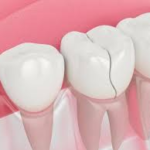
This is arguably the most common cause of bite pain without a visible cavity. A cracked tooth may have a fracture so tiny that it doesn’t appear on a standard X-ray. But when you bite down, the crack flexes, irritating the nerve inside.
What it feels like: A sharp, sudden pain when you bite into something hard, especially when you release the bite. The pain may come and go and can be difficult to pinpoint to a specific tooth.
How it’s treated: Depending on the severity, treatment ranges from a dental crown to protect the tooth, to root canal therapy if the crack has reached the pulp, to extraction in severe cases.
2. A High or Misaligned Filling
If you’ve recently had a filling placed and the biting surface is even slightly too high, it creates an uneven contact point. Every time you close your mouth, that one tooth absorbs more force than it should. Over days and weeks, this leads to persistent soreness and sensitivity.
What it feels like: A dull ache or pressure that gets worse throughout the day, especially after meals. You may feel like your bite is “off.”
How it’s treated: A quick bite adjustment at your dentist’s office. The filling is reshaped in minutes, and the relief is usually immediate.
3. Bruxism (Teeth Grinding or Clenching)
Many people grind or clench their teeth during sleep without realizing it. The constant pressure damages the periodontal ligament — the tiny cushion that holds each tooth in its socket — making teeth tender and sore when you bite.
What it feels like: Generalized soreness across several teeth, often worse in the morning. You may also notice jaw stiffness, headaches, or flat-looking tooth surfaces.
How it’s treated: A custom-fitted night guard protects your teeth from grinding forces. Your dentist may also evaluate your bite and recommend stress management techniques.
4. An Infected or Dying Nerve (Pulpitis)
Sometimes the nerve inside a tooth becomes inflamed or begins to die due to old trauma, a deep filling, or repeated dental procedures on the same tooth. The tooth may look perfectly healthy on the outside, but internally, the pulp is under distress.
What it feels like: A deep, throbbing ache that lingers after biting, or spontaneous pain that wakes you up at night. Hot and cold foods may also trigger prolonged discomfort.
How it’s treated: Root canal therapy removes the damaged nerve tissue, eliminates the infection, and saves the tooth. A crown is typically placed afterward for protection.
5. Gum Disease (Periodontal Issues)
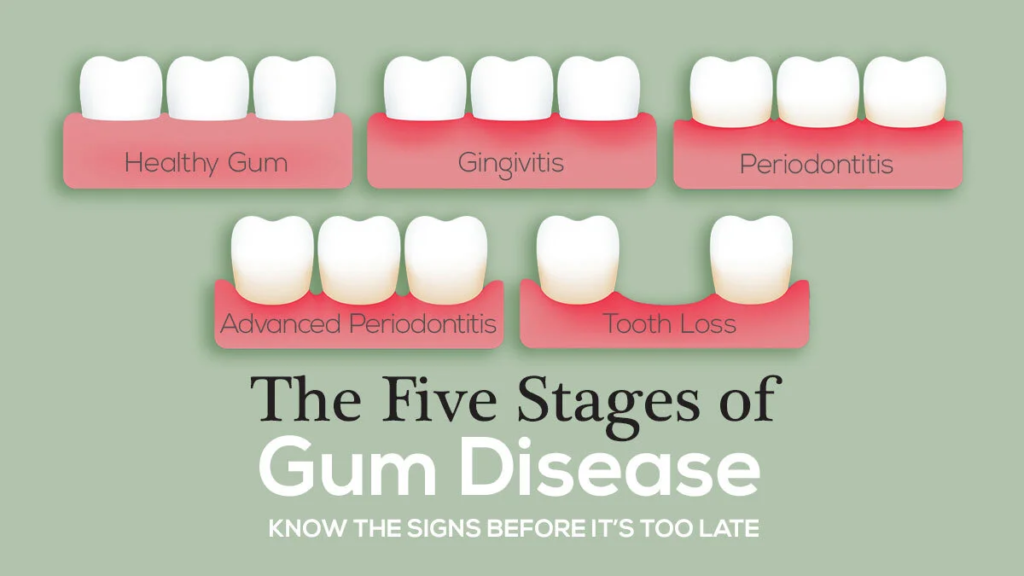
Advanced gum disease can cause the bone and tissue supporting a tooth to weaken. When you bite, the tooth may shift slightly in its compromised socket, causing pain that mimics a toothache but actually originates from the gums and bone.
What it feels like: A dull, pressure-like pain when chewing, often accompanied by gum swelling, bleeding, or a feeling that the tooth is slightly loose.
How it’s treated: Deep cleaning (scaling and root planing), improved oral hygiene, and in some cases, surgical intervention to restore gum and bone health.
6. Referred Pain from the Sinuses or TMJ
Your upper back teeth sit directly beneath your sinus cavities. When sinuses are inflamed — due to allergies, a cold, or a sinus infection — the pressure can radiate downward and feel exactly like a toothache. Similarly, TMJ disorders can cause pain that refers to specific teeth.
What it feels like: Multiple upper teeth feel sore simultaneously, especially when bending forward or when sinuses are congested. TMJ-related pain may also involve jaw clicking or stiffness.
How it’s treated: Treating the underlying sinus condition resolves the tooth pain. For TMJ issues, your dentist may recommend a bite splint, physical therapy, or other targeted treatments.
When Should You See a Dentist?
If your tooth pain when biting persists for more than a few days, don’t wait for it to go away on its own. Pain is your body’s way of telling you something needs attention. Even if X-rays appear normal, an experienced dentist can use additional diagnostic tools — bite tests, transillumination, cold tests, and 3D imaging — to uncover the cause.
At Lebanon Dental Studio, Dr. Rita Kanbar takes a thorough, diagnostic-first approach to bite pain. Rather than guessing, she systematically evaluates each possible cause to find the right answer and the right treatment for you.
| Experiencing any of these symptoms? Book a consultation at Lebanon Dental Studio. Dr. Rita Kanbar and her team are here to help. Call or WhatsApp: +961 71 677261 |
